Are we “destined to be fat”?
When I look at photos of my extended family, I have to smile.
We are peas in a pod — by which I not only mean that we look alike, but also that we tend towards being smaller and rounder.
My ancestors on both sides were sturdy, stocky farmers from the rocky British highlands and the wind-scorched Eastern European plains. They endured their share of famines, as probably all of our ancestors did at one time or another.
Given my love of eating and my draft-pony physique, I used to joke that famine prevention was woven into my DNA.
I imagined my foreparents gathered around the last frozen potato or perhaps a misshapen turnip or rust-speckled cabbage, dividing it carefully into sixteenths.
“My body is afraid of starvation,” I would explain to dinner companions, cracking into another sauce-slathered rib.
It seemed logical.
After all, food was hard to get for most of human history.
My ancestors in particular came from regions that were often blanketed in ice for thousands of years. The 3% of me that is Neanderthal DNA (try it for yourself!) still roams emotionally over the icy steppes, sturdy legs a-waddlin’, looking for a mammoth to smash into an all-you-can-eat BBQ bonanza.
You’d think, then, that frequent famine in our hominid past would change our genetic expression to favor so-called “thrifty genes” — genes that helped us store fat for a rainy (or hungry) day, and slow down our metabolisms when lunch was not forthcoming.
Like squirrels storing nuts in their cheeks, our thrifty genes would slap some adipose tissue on our asses — literal saddlebags full of provisions.
The “thrifty gene” hypothesis, as it came to be known, made a lot of sense.
It had, as Stephen Colbert would say, truthiness.
Of course our bodies would be “wired” to store fat when food was abundant.
Of course our bodies would slow down metabolism during starvation. And the more famines our ancestors endured, the more “hard wired” these traits would be.
Thus, piling on extra body fat seemed like an inevitable outcome for humanity once cheeseburgers and Doritos were invented.
(By the way, in this article I’m making no judgements about body fat — here, I use “obesity” to describe a relatively well-agreed-upon definition of having a particular percentage of adiposity. I’ll discuss whether such adiposity is a good thing elsewhere.)

Image source: ScienceNews
But there are a few problems with the “thrifty gene” idea.
As many “truthy” things often are, the “thrifty gene” hypothesis may be wrong.
Or at least, not the whole story.
My body may be no more “wired” for famine prevention — or preventive padding against the Siberian winters — than anyone else’s.
Recent research is poking some holes in the “thrifty gene” hypothesis.
(I’m only going to touch on a few things. I’m sure a qualified researcher in this field could destroy the “thrifty gene” idea and splain the whole situation much better than I. Just get the general idea here.)
Problem 1: Everyone isn’t obese.
In the 21st century industrialized world, we all live in the same environment, more or less.
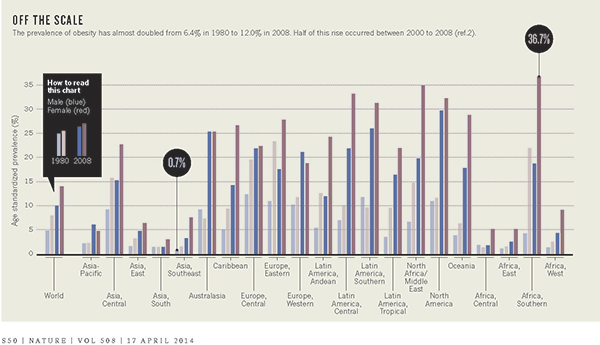
Obesity rates are going up fast. Most of us are carrying around a lot more body fat than our great-grandparents did.
But not everyone is obese.
Even in regions such as the United States where most people are now overweight, there are some people who are not obese or even overweight.
Why not?
If famine and food shortages affected nearly everyone in human history at some point, surely almost all of us should carry “thrifty genes” that store nutrients and slow down our metabolic rate.
Anyone who didn’t have these “thrifty genes” should probably have died out, right?
What gives?
In fact, you could probably make an equivalent argument for “efficiency genes” — that some people are “destined” to be lean. And perhaps you could even propose that most of us have these “efficiency genes” that kick in whenever we are living in rural, foraging, high-physical-activity situations.
Problem 2: Obesity is genetic, but complex.
Obesity probably has a genetic component.
Though estimates vary, our best guess right now is that about 65% of obesity can be explained by genetic factors.
Twin studies, for instance, show that even twins raised apart are still likely to have similar body weights and levels of body fat… unless there are significant differences in one twin’s activity or eating habits. (More on this in a moment.)
And some relatively rare genetic disorders such as Prader-Willi Syndrome can, indeed, cause lifelong adiposity combined with roaring appetite (aka hyperphagia), a situation that cruelly evokes Dante’s Third Circle of Hell where gluttons are punished mercilessly.
Note: relatively rare. Estimates of the prevalence of PWS range from 1 in 15,000 to 1 in 30,000 births for PWS. In other words, between 0.006 and 0.003% of people. Same is true for other things like leptin receptor deficiency. Given that the Centers for Disease Control estimate that currently about 35% of the US population is obese, we can safely say there are still some missing numbers.
But the more we explore the human genome as well as the field of epigenetics, the more complicated things get.
Although obesity clearly has a physiological component, in most cases there is no single “obesity gene” just like there is no single “running fast gene”.
One place we can look for genetic causes of obesity is in single nucleotide polymorphisms (SNPs).
One large study, the Genetic Investigation of Anthropometric Traits (GIANT) examined SNPs in 123,865 individuals and identified 32 important SNPs for obesity. These SNPs had large effect sizes — they noticeably affected Body Mass Index (BMI) by up to 500 grams each, or about a pound.
That sounds like a lot, especially since the SNPs seemed to be completely independent and additive. (In other words, if you had two of the SNPs, and each one told your body to be 100 grams heavier than average, you’d likely be 200 grams heavier than average.)
But even though they had significant effects on BMI, and even though their effect was cumulative, together, these SNPs together explained only 7% of the variance in BMI.
Researchers speculate that there are probably another 200 or so SNPs with similar effect sizes and there are probably hundreds to thousands of other loci each contributing around less than 100 grams per allele.
So let’s recap:
- One large-scale study found 32 SNPs with significant effects that accounted for 7% of variation in BMI.
- There are maybe about 200 more SNPs with the same significant effects, which we haven’t yet found.
- Plus, there are probably hundreds to thousands more SNPs with tiny yet meaningful effects.
That adds up to a lot of genes.
In addition, researchers speculate that many of the obesity-related genes conferred only about a 1.5% better famine survival chance.
I don’t know about you, but “You have a 1.5% better chance than your neighbor of surviving this zombie apocalypse” does not fill me with confidence. It’s sorta like “This plane is 2% less likely to crash than the other one about to go down in flames.”
Another messy bit: Most deaths in famines don’t come from starvation — they come from disease.
It’s actually pretty darn hard to die from pure, unadulterated starvation. Usually something else will nail you first. So having genes to survive plain old starvation may not help you all that much in an immediate or evolutionary sense.
Problem 3: Obesity is also epigenetic… and still complex.
Another monkey wrench in the works concerns the role of epigenetics, or the ways in which our genes can be expressed (or not).
If you’re not overly sciencey you can think of epigenetics as switching things on or off, like a light switch.
Just because we have genes doesn’t mean those genes will be expressed. Or, other factors can affect exactly how those genes get expressed.
For instance, what your mother ate, did, and/or felt before and during her pregnancy can affect your weight and metabolic health.
A fascinating example of this is the Dutch Hunger Winter of 1944, in which millions of Dutch people living in German-occupied regions were cut off from food and supplies. About 20,000 people died.
Later research discovered: If you were born to a Dutch mother who survived this stressful event, you’re more likely going to be obese and have other metabolic disruptions such as Type 2 diabetes or cardiovascular disease.
Other research also shows that stressed mothers, mothers with poor diets, and/or mothers with metabolic health problems (such as Type 2 diabetes) can “switch” the “genetic programming” of their children. Fathers, you’re not off the hook — you can also contribute.
(This doesn’t mean it’s all about blaming your parents, just that genetics alone don’t tell the whole story. But feel free to tell your therapist about the injustice of it all, if you like.)
By the way, the Dutch have also progressed from being one of Europe’s shortest populations to one of its tallest, and other populations have changed over the last few centuries too.
Problem 4: It’s not just about how much fat you might store… but where and why.
Body fatness isn’t a one-size-fits-all prescription. (See what I did there?)
Look around next time you’re in a gym locker room.
Notice how different people put on fat in different places: butts, bellies, boobs, back of arms, thighs, upper back, around their faces… Some folks have more under-the-skin fat (subcutaneous) while others have more visceral (around the internal organs) fat.
Where you put on fat is shaped by sex, genetics/epigenetics, and ethnicity (for instance, South Asians likely have more visceral fat than Europeans at the same body weight), but also by your hormones and how old you are.
Additionally, some diseases can cause lipodystrophies, basically weirdnesses in where fat gets deposited. (If you’re noticing some upper back fat, get yourself a cortisol test ASAP.)
So, past a certain point, the absolute amount of body fat is important, but so is its distribution (and the reasons why it’s there).
Just like with real estate, when it comes to adiposity and health (or mobility), it’s location, location, location.
Problem 5: Organisms seem to have upper limits of weight.
It’s actually more difficult than you’d expect to purposely make most humans and other animals obese.
Researchers have tried overfeeding people and animals. If the research subjects gain weight, they either eventually lose all or much of it. Or gear up metabolism and activity level to ditch the extra energy as heat and waste.
As one systematic review remarks, “Overfeeding studies indicate 96% less weight gain than expected if no compensation occurred.”
Organisms neither gain nor lose weight in nice, tidy mathematical ways. (So if you’re trying to do that whole imaginary linear “lose 1 lb a week” thing, you’re in for some disappointment.)
Like everything in biology, adiposity / weight has a “sweet spot”.
You want enough to keep the hormone factory and immune system working — enough to tell the body that things are A-OK. But you don’t want so much that it impedes your mobility and function.
So our bodies prefer to keep adiposity and weight within a happy range. Not too much, not too little.
Of course, as per points #1-4, not everyone responds to overfeeding in the same way.
With me so far?
So at this point we have:
- Some people are obese. But some are not.
- Genetics matter, but it’s complicated.
- Epigenetics also matter, and it’s also complicated.
- It’s not just about how much fat, but where it goes and why it’s there. Again, complicated.
- For most people, past a certain point, it’s hard to put on a lot of weight on purpose.
OK, good.
Well, that’s nice and messy and unhelpful.
Environment matters.
If about 65% of obesity can be explained by genetic factors of some kind, then about 35% of obesity (or body weight in general) can be explained by other things.
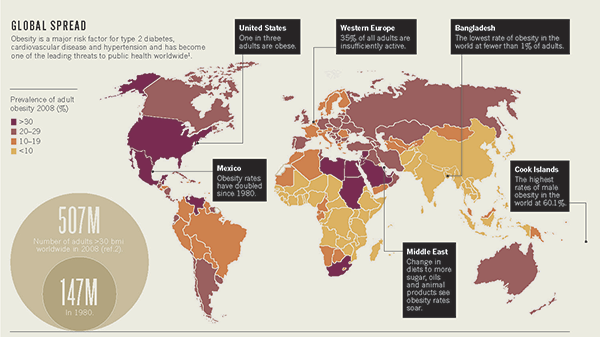
If you look at the map of where and how obesity is distributed, it’s pretty clear that there must be other factors involved.
For instance, most of sub-Saharan Africa along with southern and eastern Asia has relatively low rates of obesity.
However:
- People of African descent living in the United States are more likely to be overweight or obese.
- Immigrants arriving in North America often start putting on weight soon after arrival (and if they don’t, their kids usually do).
- In affluent countries, poverty often means excess body weight; in poorer countries the reverse is true.
Are poor people genetically different than rich people? (And do they swap genes in different countries?)
Is a subsistence farmer in Nicaragua, Sudan, or Bangladesh somehow equipped with special DNA (which they then lose when they migrate to North America)?
Of course not (although one could reasonably make an argument in favour of stress affecting epigenetic expression of people who are socially marginalized, such as African Americans).
Environments can dramatically affect our health and choices.
And much of our environment is not under our control.
For instance, people can’t necessarily control things like:
- Light and dark cycles (or having a job where our light and dark cycles get messed up)
- Infrastructure and access to resources (like fresh, clean running water)
- What food is available (or not)
- Environmental stressors (such as social and physical stress, etc.)
However, if you’re reading this on a computer, you are probably richer than the vast majority of the world’s population.
That means you may have some individual control over your environment and your choices.
If we look at who’s been successful at maintaining a healthy weight, even when they’re surrounded by the obesegenic shit-show that is 21st century industrialized culture:
- They’re active.
- They’re mindful about what they eat.
- They stay honest and aware of their health, activity, and food intake (without getting psycho about it).
Note that this is a healthy weight.
Not “lean” necessarily. Perhaps even a little squishy.
But nevertheless a weight that contains a robust proportion of lean body mass (strong, dense muscle, connective tissues, and bone) and allows people to do whatever they need and want to do.
What this all means
We don’t completely understand why people are the way they are. We can only make some educated guesses.
Many factors interact to influence body shape and size. Again, we probably don’t know all of the factors, nor do we fully understand the ones we do know about.
Body shape and size is not either-or. It’s not nature or nurture. It’s both, and some other stuff too. You are not “doomed” to be anything in particular and at the same time there are many factors that strongly affect how your body looks, feels, and behaves.
Many factors are, to some degree, under your control. You’re a sculptor, and ya gotta work the clay you got… but it’s usually reasonably malleable.
If your genetic machinery was totally fucked up, you wouldn’t be alive right now. The fact that you have survived and are reading this deserves a high-five. That means most of your stuff is awesome. And at least something about you is negotiable, if you want it to be.
Blaming people, getting all lecture-y on them, or suggesting that they have “failed” or “made excuses” for whatever shape and size they are is fucking stupid and insensitive. If that’s you beaking off about “no excuses” for not having abs, please shut the fuck up.
There’s a “sweet spot” for your species… and for you personally. Whatever that physiological sweet spot of adiposity and weight is for you, find it and thrive in it.
You don’t have to be a superhero. Just take care of yourself. Stay moving. Be aware of what you’re putting in your body. Treat yourself with love.
References
Beil, Laura. Ancient famine-fighting genes can’t explain obesity. ScienceNews September 5, 2014.
Catenacci VA, et al. Physical activity patterns in the National Weight Control Registry. Obesity 16 no.1 (January 2008): 153-161.
Dhurandhar EJ, et al. Predicting adult weight change in the real world: a systematic review and meta-analysis accounting for compensatory changes in energy intake or expenditure. International Journal of Obesity (December 2014).
Garland, Theodore et al. The biological control of voluntary exercise, spontaneous physical activity and daily energy expenditure in relation to obesity: human and rodent perspectives. The Journal of Experimental Biology 214 no.2 (2011):206-229.
Genné-Bacon, Elizabeth A. Thinking evolutionarily about obesity. Yale Journal of Biology and Medicine 87 no.2 (June 2014): 99-212.
Hebebrand Johannes, et al. Molecular genetic aspects of weight regulation. Deutsche Arteblatt International 19 (May 2013):338-44.
Hinney, Anke, et al. From monogenic to polygenic obesity: recent advances. European Child and Adolescent Psychiatry 19 no.3 (March 2010): 297-310.
Jakicic JM, Davis KK. Obesity and physical activity. Psychiatric Clinics of North America. 34 no.4 (December 2011): 829-840.
Klem, Mary L., et al. A descriptive study of individuals successful at long-term maintenance of substantial weight. American Journal of Clinical Nutrition 66 (l997): 239-46.
Stehr MD, von Lengerke T. Preventing weight gain through exercise and physical activity in the elderly: a systematic review. Maturitas 72 no.1 (May 2012): 13-22.
Santarpia L, et al. Body composition changes after weight-loss interventions for overweight and obesity. Clinical Nutrition 32 no.2 (April 2013): 157-161.
Speakman, John R. and Klaas R. Westerterp. A mathematical model of weight loss under total starvation: evidence against the thrifty-gene hypothesis. Disease Models and Mechanisms 6 no.1 (Jan 2013): 236–251.
Speakman, John. Thrifty genes for obesity and the metabolic syndrome – time to call off the search? Diabetes & Vascular Disease Research 3 (2006):7–11.
Strasser, Barbara. Physical activity in obesity and metabolic syndrome. Annals of the New York Academy of Sciences. 1281 no.1 (2013): 141–159.
Tappy, Luc. Metabolic consequences of overfeeding in humans. Current Opinion in Clinical Nutrition & Metabolic Care 7 no.6 (November 2004): 623-628.
Wells, Jonathan C.K. Ethnic variability in adiposity and cardiovascular risk: the variable disease selection hypothesis. International Journal of Epidemiology 38, no.1 (2008): 63-71.
Willyard, Cassandra. The family roots of obesity. Nature 508 (April 2014): S58-S60.
Wing, Rena R. and Suzanne Phelan. Long-term weight loss maintenance. American Journal of Clinical Nutrition 82 no.1 (July 2005): 2225-2255.